Through collaboration with rural communities and practices, the iCARE project provides clinical services and practice support with a focus on innovative technologies. iCARE supports rural clinical practices through onsite primary care and subspecialty support, telemedicine, technical skills training, and community engagement.
Transportation barriers can be an impediment for rural residents with specialty care needs. This program provides boots-on-the-ground subspecialists, including pediatric subspecialists, maternal-fetal medicine specialists, psychiatry specialists, and adult cardiologists, to augment the care being provided in the local community. Clinicians also use telehealth or innovative models to expand local clinical services in rural communities.
iCARE Funding Opportunity
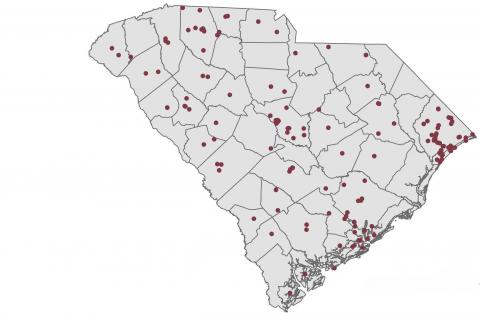
Map of Active iCARE projects